Have you changed your mind about having children and need to know if vasectomies can be reversed? Vasectomy reversals are microsurgical procedures to rectify the effects of a vasectomy. A vasectomy is a contraceptive method to prevent pregnancies while having sexual intercourse. However, you and your partner may decide to have a vasectomy reversal if you want to have children and start your family.

(Source)
It is an important life decision that requires careful planning and consideration. While it is a relatively straightforward procedure, it comprises some of the most complex and intricate microsurgical procedures. Therefore, it is essential to know what happens during the process beforehand.
What to Know Before a Vasectomy Reversal?
One of the first things that your surgeon will do is make sure that none of your previous medical history, conditions, diseases, or disorders interfere with the procedure and complicate it. After reviewing your medical history, the doctor/surgeon will do a sperm analysis.
This analysis saves your time and trouble of getting into a vasectomy reversal if your body is unable to produce healthy and fertile sperm. Hence, there may not be chances of pregnancy from the start. However, if the reports reveal the production of healthy sperm, the surgeon will carry on with further questions and inquiries.
Your partner will also undergo tests and analysis to make sure that she can conceive and form embryos. Old age complicates the reversal procedure, so chances of conceiving significantly reduce with reverse vasectomy when a man/woman ages.
During the Microsurgery Procedure – Vasectomy Reversal
You will have your vasectomy reversal process on an outpatient basis which doesn’t require a long hospital stay.
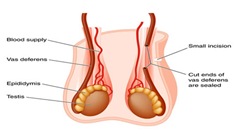
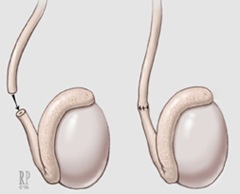
At your surgeon’s discretion, you will receive either local or general anesthesia. Then the procedure begins with the surgeon making an incision on your scrotum, which reveals the vas deferens. These tubes carry the sperm from the male reproductive organs (testes) to the urinary/ejaculatory duct.
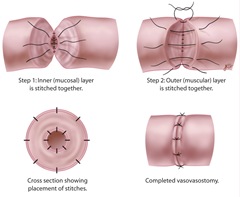
Gently handling the vas from your scrotum, the surgeon will make minor incisions to test if fluid is present in the vein. In case there is water/clear fluid and sperm, the surgeon will carry out a vasovasostomy.
Re-attachment of the severed ends will occur, ensuring the restoration of the pathway for sperms to move from the testes to the penis.
In the case of a dry vas or the lack of sperm in the fluid that may be present in the vas, the surgeon will carry out an epididymovasostomy. This method allows the surgeon to attach one end of the vas directly to the epididymis on the testes.
Note that these are microsurgeries that are complex and much more intricate than a vasectomy itself. In order to perform such an operation, the surgeon will use a microscope, microsurgical instruments, and other precision equipment.
After the Procedure
It can take nearly four weeks for the veins (vas deferens) to heal or more in some cases. It is also possible that your surgeon might perform vasovasostomy on one vas and epididymovasostomy on the other one. Moreover, you should not let your bandages and stitches come in contact with water or anything wet for at least two days/48 hours.
Furthermore, it is advisable to avoid heavy lifting, aerobic exercises, and, more importantly, sexual intercourse for two weeks after the procedure. Using ice packs, antibiotics, painkillers, and other medication can help take care of any bruising, swelling, or pain.
Chances of Pregnancy
Once the procedure takes place, pregnancy might not occur instantly. It can take time for the sperm to get back into the tubes and start mixing with the semen. In reality, sperm carrying ejaculate can form over the course of nearly 4-6 months. Meanwhile, your surgeon will take semen samples to ensure that sperms are healthy and fertile while also capable of mobility.

(Source)
Pregnancy rates may not be 100 or 99 percent, but they are significantly higher, which is around 60-90 percent on average. Additionally, it is best to consult your doctor or surgeon in case of any unexpected emergencies after the procedure or side effects.
Can Vasectomies Be Reversed: Conclusion
Do you want to consult with one of the best urologists and vasectomy reversal experts? Dr. Yaniv Larish is a urologist and expert in performing microsurgery, especially vasectomy reversals. With extensive experience in the medical process, he can guide you and ensure the effective completion of the procedure.
Give us a call at (646) 862-5500 to schedule a consultation with Dr. Larish today. Visit us at 4 East 76th Street New York, NY 10021 for in-person inquiries. Vasectomy reversals are a sensitive concern and demand high-level expertise and skills for success.
Yaniv Larish, MD
4 East 76th Street
New York, NY 10021
(646) 862-5500
Reference Links
https://www.mayoclinic.org/tests-procedures/vasectomy-reversal/about/pac-20384537
https://urologyaustin.com/male-urology/preparing-for-a-vasectomy-reversal/
https://clearpointhealth.ca/blog/5-facts-you-should-know-before-your-vasectomy-reversal/
https://myhealth.alberta.ca/Health/aftercareinformation/pages/conditions.aspx?hwid=zc2385


 Vasectomy reversal vs. donor sperm is a common comparison for couples exploring fertility options after a prior vasectomy. Both paths can lead to parenthood, but they involve very different medical, emotional, and financial considerations. Understanding how these approaches differ can help couples decide which option best aligns with their goals, timeline, and personal preferences.
Vasectomy reversal vs. donor sperm is a common comparison for couples exploring fertility options after a prior vasectomy. Both paths can lead to parenthood, but they involve very different medical, emotional, and financial considerations. Understanding how these approaches differ can help couples decide which option best aligns with their goals, timeline, and personal preferences.

 What should you expect during a vasectomy reversal procedure? Vasectomy reversal is a highly specialized microsurgical procedure designed to restore fertility in men who have previously undergone a vasectomy. Whether due to changing life circumstances, a new relationship, or a desire to expand one’s family, vasectomy reversal offers hope to men seeking to father children again. Understanding the details of the procedure can help patients feel more confident about the process and what to expect.
What should you expect during a vasectomy reversal procedure? Vasectomy reversal is a highly specialized microsurgical procedure designed to restore fertility in men who have previously undergone a vasectomy. Whether due to changing life circumstances, a new relationship, or a desire to expand one’s family, vasectomy reversal offers hope to men seeking to father children again. Understanding the details of the procedure can help patients feel more confident about the process and what to expect.