Let’s explore the advantages and considerations of vasectomy reversal vs. IVF, helping you make an informed decision about the best route for your family planning goals. For men who have previously undergone a vasectomy but now wish to father children, two primary options exist: vasectomy reversal and in vitro fertilization (IVF). Both methods offer a pathway to conception, but they differ significantly in approach, cost, success rates, and long-term impact.
Let’s explore the advantages and considerations of vasectomy reversal vs. IVF, helping you make an informed decision about the best route for your family planning goals. For men who have previously undergone a vasectomy but now wish to father children, two primary options exist: vasectomy reversal and in vitro fertilization (IVF). Both methods offer a pathway to conception, but they differ significantly in approach, cost, success rates, and long-term impact.
Understanding Vasectomy Reversal
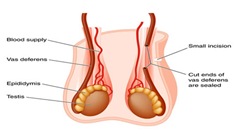
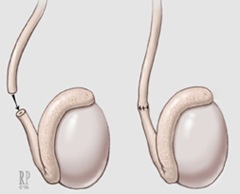
Vasectomy reversal is a microsurgical procedure that reconnects the vas deferens, the tubes that transport sperm from the testicles to the urethra. This procedure allows for the return of sperm to the ejaculate, restoring the ability to conceive naturally.
The procedure is performed using highly advanced techniques to ensure precision and minimize tissue damage. Success rates vary based on factors such as the length of time since the vasectomy and the presence of blockages, but many men regain their fertility and successfully conceive.
The Role of Microsurgery in Fertility Restoration
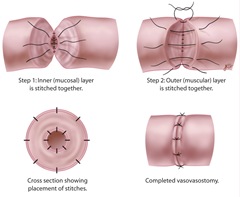
Vasectomy reversal is a delicate procedure that relies on microsurgical techniques to achieve optimal outcomes. This involves using specialized instruments and a high-powered surgical microscope to ensure a precise reconnection of the vas deferens.
- Microsurgical Accuracy: The use of high-powered magnification enables the surgeon to make precise sutures, ensuring that the vas deferens heals properly and sperm flow is restored.
- Customized Techniques: Based on intraoperative findings, the surgeon will perform either a vasovasostomy (direct reconnection of the vas deferens) or a vasoepididymostomy (bypass of a blockage in the epididymis).
- Minimally Invasive Approach: Microsurgery reduces trauma to surrounding tissues, improving recovery time and overall success rates.
IVF as an Alternative to Vasectomy Reversal
 In in vitro fertilization (IVF), sperm is retrieved directly from the testicles through procedures like testicular sperm extraction (TESE) or percutaneous epididymal sperm aspiration (PESA). The retrieved sperm is then used to fertilize an egg in a laboratory setting, and the resulting embryo is transferred into the uterus.
In in vitro fertilization (IVF), sperm is retrieved directly from the testicles through procedures like testicular sperm extraction (TESE) or percutaneous epididymal sperm aspiration (PESA). The retrieved sperm is then used to fertilize an egg in a laboratory setting, and the resulting embryo is transferred into the uterus.
IVF bypasses the need for vasectomy reversal but comes with its own considerations:
- Assisted Reproduction: IVF requires medical intervention at multiple stages, including egg retrieval, fertilization, and embryo transfer.
- Higher Costs: IVF can be more expensive than vasectomy reversal, particularly if multiple cycles are needed.
- Hormonal Treatments: The female partner must undergo hormone therapy to stimulate egg production, which can have side effects.
- Lower Natural Conception Rates: Since IVF does not restore natural sperm flow, future pregnancies will require additional IVF cycles.
Comparing Vasectomy Reversal and IVF
Each approach has its advantages and limitations, and the choice will depend on your specific circumstances.
Key Factors to Consider:
- Success Rates: Vasectomy reversal success rates range from 40% to over 90%, depending on the time since vasectomy and other factors. IVF success rates are around 30-50% per cycle, varying based on the female partner’s age and reproductive health.
- Cost Considerations: Vasectomy reversal is typically a one-time expense, whereas IVF can require multiple cycles, significantly increasing costs.
- Natural Conception: Vasectomy reversal restores the ability to conceive naturally, while IVF requires medical intervention for each pregnancy.
- Medical Invasiveness: IVF involves hormonal treatments, egg retrieval, and embryo transfer, making it more invasive than vasectomy reversal.
What to Expect Before, During, and After Vasectomy Reversal
Vasectomy reversal is a one-time outpatient procedure with a recovery period of a few weeks. Here’s what you can expect:
Before Surgery
- Comprehensive Consultation: A detailed evaluation, including a review of medical history and fertility assessments, is conducted.
- Pre-Operative Instructions: Patients receive guidelines on medications, dietary restrictions, and preparation for surgery.
During Surgery
- Procedure Length: The surgery typically lasts 2-4 hours and is performed under general anesthesia.
- Microsurgical Technique: The surgeon makes a small incision in the scrotum, reconnects the vas deferens, and ensures proper sperm flow.
Post-Operative Recovery
- Healing Process: Most patients recover within 2-4 weeks, with mild swelling and discomfort managed by pain relievers.
- Follow-Up Care: A semen analysis is conducted 6-8 weeks post-surgery to evaluate sperm presence and quality.
When IVF Might Be the Better Option
While vasectomy reversal is the preferred option for many men, there are cases where IVF may be the better choice:
- Severe Female Fertility Issues: If the female partner has difficulty conceiving naturally due to low egg reserve or other reproductive concerns, IVF may be the recommended option.
- Time Since Vasectomy: If the vasectomy was performed more than 15-20 years ago, scar tissue and blockages may lower reversal success rates, making IVF a better alternative.
- Desire for Immediate Conception: IVF allows for fertilization and embryo transfer within a short timeframe, whereas vasectomy reversal requires a waiting period of several months before sperm production is restored.
Making the Right Choice for You
Choosing between vasectomy reversal and IVF is a personal decision that depends on your medical history, reproductive goals, and financial considerations. Consulting with a specialist can help you determine the most effective approach for achieving pregnancy.
If you’re considering vasectomy reversal or exploring fertility options, contact:
Yaniv Larish, MD
4 East 76th Street
New York, NY 10021
Phone: (646) 862-5500
Dr. Yaniv Larish specializes in microsurgical vasectomy reversals and fertility restoration. Schedule a consultation today to learn more about your options and take the next step toward parenthood.


 NYC’s most trusted surgeons for vasectomy reversal typically share several important qualities, including specialized microsurgical training, extensive experience, and a strong track record of successful outcomes. Because vasectomy reversal is a technically demanding procedure involving structures smaller than a millimeter, choosing the right surgeon can significantly influence your chances of restoring fertility.
NYC’s most trusted surgeons for vasectomy reversal typically share several important qualities, including specialized microsurgical training, extensive experience, and a strong track record of successful outcomes. Because vasectomy reversal is a technically demanding procedure involving structures smaller than a millimeter, choosing the right surgeon can significantly influence your chances of restoring fertility.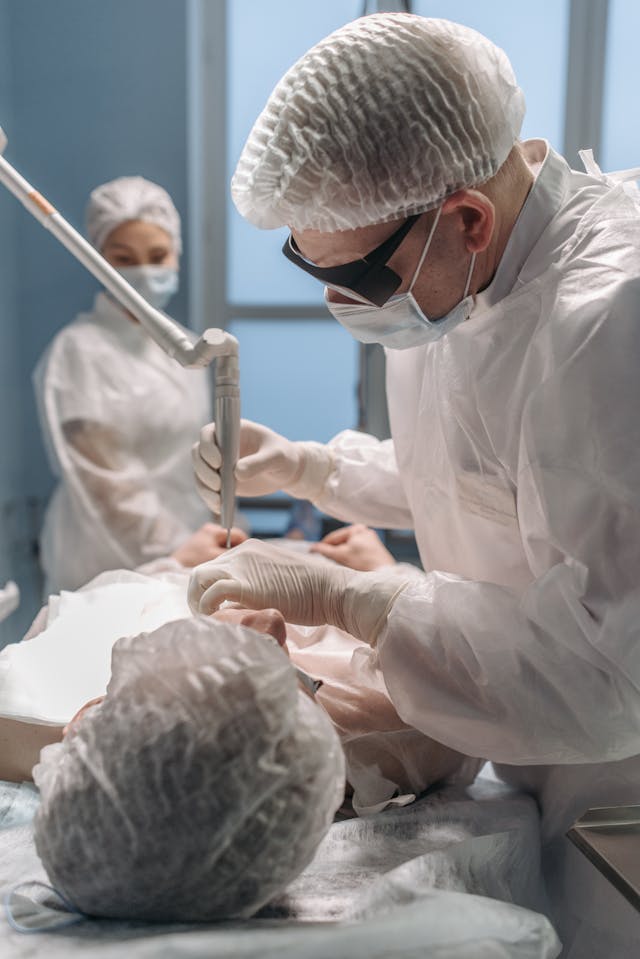 Microsurgical vasectomy reversal offers higher success rates because it allows surgeons to precisely reconnect the delicate reproductive structures involved in sperm transport. Compared with older surgical approaches, microsurgery uses advanced magnification, specialized instruments, and refined suturing techniques to maximize the chances of restoring fertility after a vasectomy.
Microsurgical vasectomy reversal offers higher success rates because it allows surgeons to precisely reconnect the delicate reproductive structures involved in sperm transport. Compared with older surgical approaches, microsurgery uses advanced magnification, specialized instruments, and refined suturing techniques to maximize the chances of restoring fertility after a vasectomy.
 Vasectomy reversal vs. donor sperm is a common comparison for couples exploring fertility options after a prior vasectomy. Both paths can lead to parenthood, but they involve very different medical, emotional, and financial considerations. Understanding how these approaches differ can help couples decide which option best aligns with their goals, timeline, and personal preferences.
Vasectomy reversal vs. donor sperm is a common comparison for couples exploring fertility options after a prior vasectomy. Both paths can lead to parenthood, but they involve very different medical, emotional, and financial considerations. Understanding how these approaches differ can help couples decide which option best aligns with their goals, timeline, and personal preferences. Understanding whether health insurance covers vasectomy reversal in New York is a common concern for men considering this procedure, as costs can influence family‑planning decisions. While vasectomy reversal is a well‑established surgical option for restoring fertility, insurance coverage varies widely and depends on your plan, provider, and policy specifics.
Understanding whether health insurance covers vasectomy reversal in New York is a common concern for men considering this procedure, as costs can influence family‑planning decisions. While vasectomy reversal is a well‑established surgical option for restoring fertility, insurance coverage varies widely and depends on your plan, provider, and policy specifics.


 For couples hoping to conceive after a vasectomy reversal, a common question is: how long will it take to achieve pregnancy? While the answer varies depending on individual factors, understanding the typical timeline and influences on success can help set realistic expectations.
For couples hoping to conceive after a vasectomy reversal, a common question is: how long will it take to achieve pregnancy? While the answer varies depending on individual factors, understanding the typical timeline and influences on success can help set realistic expectations. For men considering a return to fatherhood after a vasectomy, vasectomy reversal can offer a hopeful path to natural conception. However, deciding whether it’s the right choice depends on several medical, emotional, and lifestyle factors. If you’re in the NYC or Tri-State area and weighing your options, this guide will help you ask the right questions before committing to surgery.
For men considering a return to fatherhood after a vasectomy, vasectomy reversal can offer a hopeful path to natural conception. However, deciding whether it’s the right choice depends on several medical, emotional, and lifestyle factors. If you’re in the NYC or Tri-State area and weighing your options, this guide will help you ask the right questions before committing to surgery.
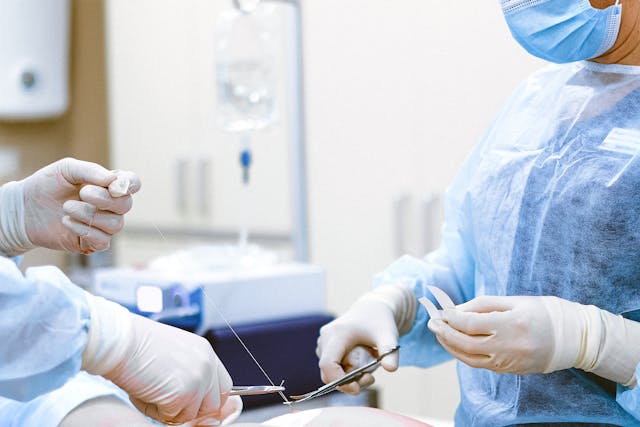

 Vasectomy reversal is a highly effective and safe procedure, yet it remains surrounded by myths and misunderstandings. These misconceptions often deter men and couples from exploring the option of restoring fertility after a vasectomy. In this blog, we’ll debunk some of the most common misconceptions about vasectomy reversal to provide clarity for those considering the procedure.
Vasectomy reversal is a highly effective and safe procedure, yet it remains surrounded by myths and misunderstandings. These misconceptions often deter men and couples from exploring the option of restoring fertility after a vasectomy. In this blog, we’ll debunk some of the most common misconceptions about vasectomy reversal to provide clarity for those considering the procedure.
 Recovery after a vasectomy reversal is a crucial phase in the journey to restoring fertility, and understanding what to expect can significantly improve healing and long-term outcomes. While the surgical procedure itself is highly specialized, the post-operative period plays an equally important role in determining success. In this blog, we’ll cover recovery timelines, self-care tips, and what to expect during each stage of healing.
Recovery after a vasectomy reversal is a crucial phase in the journey to restoring fertility, and understanding what to expect can significantly improve healing and long-term outcomes. While the surgical procedure itself is highly specialized, the post-operative period plays an equally important role in determining success. In this blog, we’ll cover recovery timelines, self-care tips, and what to expect during each stage of healing.
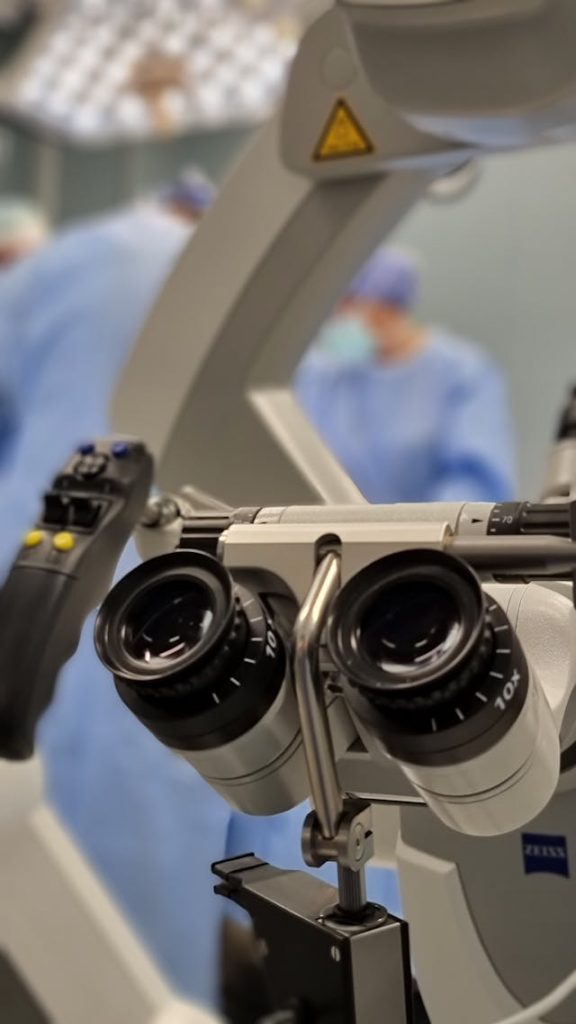 In this article we’ll explore the importance of the surgical microscope in vasectomy reversal and how it contributes to optimal patient outcomes. Vasectomy reversal is a delicate procedure that requires extreme precision to reconnect the vas deferens and restore the flow of sperm. One of the most critical tools in ensuring a successful outcome is the surgical microscope. This advanced piece of technology allows urologic
In this article we’ll explore the importance of the surgical microscope in vasectomy reversal and how it contributes to optimal patient outcomes. Vasectomy reversal is a delicate procedure that requires extreme precision to reconnect the vas deferens and restore the flow of sperm. One of the most critical tools in ensuring a successful outcome is the surgical microscope. This advanced piece of technology allows urologic 
 Let’s explore the advantages and considerations of vasectomy reversal vs. IVF, helping you make an informed decision about the best route for your family planning goals. For men who have previously undergone a vasectomy but now wish to father children, two primary options exist: vasectomy reversal and in vitro fertilization (IVF). Both methods offer a pathway to conception, but they differ significantly in approach, cost, success rates, and long-term impact.
Let’s explore the advantages and considerations of vasectomy reversal vs. IVF, helping you make an informed decision about the best route for your family planning goals. For men who have previously undergone a vasectomy but now wish to father children, two primary options exist: vasectomy reversal and in vitro fertilization (IVF). Both methods offer a pathway to conception, but they differ significantly in approach, cost, success rates, and long-term impact. In in vitro fertilization (IVF), sperm is retrieved directly from the testicles through procedures like testicular sperm extraction (TESE) or percutaneous epididymal sperm aspiration (PESA). The retrieved sperm is then used to fertilize an egg in a laboratory setting, and the resulting embryo is transferred into the uterus.
In in vitro fertilization (IVF), sperm is retrieved directly from the testicles through procedures like testicular sperm extraction (TESE) or percutaneous epididymal sperm aspiration (PESA). The retrieved sperm is then used to fertilize an egg in a laboratory setting, and the resulting embryo is transferred into the uterus.